Rocky Mountain Spotted Fever
What is Rocky Mountain Spotted Fever?
Rocky Mountain Spotted Fever (RMSF) is a severe disease caused by tick bites in the United States. A majority of RMSF cases in Arizona happen in communities with large number of roaming dogs and a lot of ticks. The first case of RMSF was in 1896 in Snake River Valley, Idaho; however, Arizona has the most cases of RMSF in the US. Rocky Mountain spotted fever is more common in the south Atlantic and south central parts of the United States then it is in the Rocky Mountains.
Rocky Mountain spotted fever (RMSF) can be fatal within the first few days of symptoms if not treated correctly, even in previously healthy people. It is caused by the bacterium Rickettsia rickettsii and is transmitted to humans by the bite of infected ticks. In the United States, these include the American dog tick (Dermacentor variabilis), Rocky Mountain wood tick (Dermacentor andersoni), and brown dog tick (Rhipicephalus sanguineus). The brown dog tick and other tick species are also associated with RMSF in Central and South America. The tick bite is usually painless and about half of the people who develop RMSF do not remember being bitten.
Rickettsia rickettsii infects the endothelial cells that line the blood vessels. The damage that occurs in the blood vessels results in a disease process called a “vasculitis”, and bleeding or clotting in the brain or other vital organs may occur. In severe cases, loss of fluid from damaged vessels can result in loss of circulation to the extremities and damaged fingers, toes or even limbs may ultimately need to be amputated. Patients who suffer this kind of severe vasculitis in the first two weeks of illness may also be left with permanent long-term health problems such as profound neurological deficits, or damage to internal organs. Those who do not have this kind of vascular damage in the initial stages of the disease typically recover fully within several days to months.
In addition to Rickettsia rickettsii, the agent of Rocky Mountain spotted fever (RMSF), several other tick-borne species of Rickettsia, broadly grouped under the heading “Spotted Fever Group Rickettsia (SFGR)” have been shown to cause human infections.
Is Rocky Mountain Spotted Fever in Colorado?
Rocky Mountain Spotted Fever (R. rickettsii) is known to occur in Colorado and may be transmitted through the bite of the Rocky Mountain wood tick (Dermacentor andersoni), the American Dog tick (Dermacentor variabilis) or the Brown dog tick (Rhipicephalus sanguineus). Contrary to what the name suggests, this disease is more prevalent outside of the Rocky Mountain region, and is considered rare in Colorado.
What are Rocky Mountain Spotted Fever Symptoms?
Few people with the disease will develop all symptoms, and the number and combination of symptoms varies greatly from person to person. It is a multi-systemic disease and potentially severe, and may affect the central nervous system, respiratory system, gastric system and renal system. Neurologic manifestations include meningitis, cranial neuropathies, deafness, paralysis, spasticity, vertigo, aphasia and photophobia. Pulmonary involvement includes edema, pneumonia and respiratory distress syndrome. Microcirculatory vasculitis can lead to myocarditis. Ophthalmologic complications can also occur. Hospitalization is frequently required in advanced cases of RMSF.
The first symptoms of Rocky Mountain spotted fever (RMSF) typically begin 2-14 days after the bite of an infected tick and may include:
- Fever
- Rash (occurs 2-5 days after fever, may be absent in some cases)
- Headache
- Nausea
- Vomiting
- Abdominal pain (may mimic appendicitis or other causes of acute abdominal pain)
- Muscle pain
- Lack of appetite
- Red eyes
- Lethargy
- Confusion
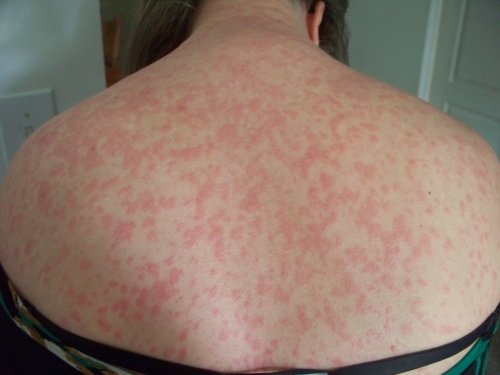
Rash
The “classic” RMSF rash, consisting of small, bright red or pink flat, non-itchy petechial (spotted) lesions, on the wrists, forearms, and ankles and spreads to include the trunk and sometimes the palms and soles, does not usually appear until almost a week after symptom onset. Estimates vary as to its prevalence, with most sources stating that it presents eventually in about half of all RMSF patients.
Close to 5% of patients will develop gangrene or skin necrosis, sometimes requiring amputation of the affected extremities. While most people with RMSF have some type of rash during the course of illness, some people do not develop the rash until late in the disease process (after treatment should have been initiated), and others never develop a rash. People who fail to develop a rash, or develop an atypical rash, are at increased risk of being misdiagnosed.
Children
Children with RMSF infection may experience nausea, vomiting, and loss of appetite. Children are less likely to report a headache, but more likely to develop an early rash than adults. Other frequently observed signs and symptoms in children with RMSF are abdominal pain, altered mental status, and red eyes. Occasionally, symptoms like cough, sore throat, and diarrhea may be seen, and can lead to misdiagnosis.
How is Rocky Mountain spotted fever Diagnosed?
Per the CDC, “The diagnosis of RMSF must be made based on clinical signs and symptoms, and can later be confirmed using specialized confirmatory laboratory tests. Treatment should never be delayed pending the receipt of laboratory test results, or be withheld on the basis of an initial negative finding for R. rickettsia.”
Healthcare providers must use their judgment to treat patients based on clinical suspicion alone. Information such as recent tick bites, exposure to high grass and tick-infested areas, contact with dogs, similar illnesses in family members or pets, or history of recent travel to areas of high incidence can be helpful in making the diagnosis.
Routine blood tests, such as a complete blood cell count or a chemistry panel may assist in diagnosis. Clues, such as a low platelet count (thrombocytopenia), low sodium levels (hyponatremia), or elevated liver enzyme levels may be predictors of RMSF, but may not be present in all patients. Prompt treatment with doxycycline is recommended if RMSF is suspected, and should never be delayed pending the outcome of diagnostic tests.
Diagnostic tests for this disease, especially tests based on the detection of antibodies, will frequently appear negative in the first 7-10 days of illness. Due to the complexities of this disease and the limitations of currently available diagnostic tests, there is no test available at this time that can provide a conclusive result in time to make important decisions about treatment. If disease is suspected, treatment should be initiated immediately.
How do you test for Rocky Mountain Spotted Fever?
The disease frequently begins as a sudden onset of fever and headache. Because early symptoms may be non-specific, several visits to a physician may occur before the diagnosis of RMSF is made and correct treatment begins. The clinical presentation for RMSF can resemble other tick-borne diseases, such as Ehrlichiosis and Anaplasmosis. Similar to RMSF, these infections respond well to treatment with doxycycline.
- Blood specimens (whole blood, serum) are not always useful for detection of the organism through polymerase chain reaction (PCR) or culture. R. rickettsii infects the endothelial cells that line blood vessels, and does not circulate in large numbers in the blood unless the patient has progressed to a very severe phase of infection.
- PCR or immunohistochemical (IHC) staining can be performed on a skin biopsy taken from the rash site. This test can often deliver a rapid result, however a negative result should not be used to guide treatment decisions. Culture of R. rickettsii is only available at specialized laboratories; routine hospital blood cultures cannot detect R. rickettsii.
- Indirect immunofluorescence assay (IFA) with R. rickettsii antigen is the gold standard serologic test for diagnosis of RMSF. It is performed on two paired serum samples to demonstrate a significant (four-fold) rise in antibody titers and can be used to confirm diagnosis after treatment has been initiated.
How is Rocky Mountain Spotted Fever treated?
Treatment for this disease is most effective at preventing serious complications or death if started in the first five days of symptoms. Patients who are treated early may recover quickly on outpatient medication, while those who experience a more severe course may require intravenous antibiotics, prolonged hospitalization or intensive care. Treatment should never be delayed pending confirmation of laboratory tests!
Per the CDC, “Doxycycline is the first line treatment for adults and children of all ages and should be initiated immediately whenever RMSF is suspected.”
*Pregnant women or those with life threatening allergies to Doxycycline may be treated with chloramphenicol.
References
2020 Rickettsiosis Subcommittee Report to the Tick-Borne Disease Working Group
Columbia University Medical Center-Lyme and Other Tick-borne Diseases Research Center