Diagnosing Lyme Disease
Diagnosing Lyme
Lyme disease is a clinical diagnosis
According to the CDC, a diagnosis of Lyme disease should be based on symptoms. If you have symptoms of Lyme disease you may be infected, even if your blood test is negative.
It can be especially challenging for Coloradans to receive accurate diagnosis and effective treatment for Lyme and potential co-infections. Many Colorado physicians are not experienced at recognizing the many manifestations of Lyme and co-infections. They may not consider Lyme in the differential diagnosis, especially if their patient has not recently travelled to a known endemic area, or if they do not recall a tick bite. The belief that “Lyme does not exist in Colorado” often inhibits timely diagnosis and treatment for patients regardless of where they may have been exposed.
It is important for Coloradans who are affected by Lyme disease to be aware of the controversy around diagnosis, testing and treatment so they can make informed choices about their health care. Medical professionals both in Colorado and nationwide approach the diagnosis and treatment of Lyme disease in different ways.
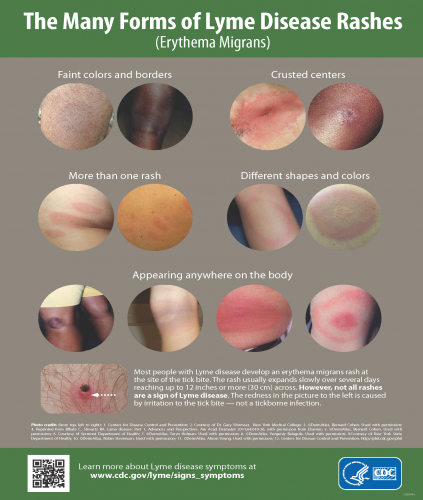
Some professionals and institutions believe that a “Bull’s eye” (Erythema Migrans) rash, or a CDC surveillance criteria positive blood test must be present to diagnose Lyme disease.
Not Everyone Gets a “Bull’s-Eye” Rash
The CDC states that 20%-30% of people with Lyme disease never get a bull’s-eye rash. Physicians that routinely treat Lyme disease are observing that this number is even greater, in nearly 50% of their Lyme patients a rash is absent. Atypical rashes are common and an often overlooked symptom as well. Skin tone may also affect presentation or recognition of rash.
Blood tests for Lyme disease can be inaccurate
Blood tests for Lyme disease and co-infections may result in false negatives and false positives, and tests are not always available for some of the co-infections that may appear as a co-infection with Lyme.
Due to lack of reliable direct testing methods, diagnosis may be supported by laboratory testing but, cannot be “ruled out” through negative test results.
There are several laboratories that specialize in the testing for Lyme and other tick-borne diseases.
Varied presentations of Lyme disease
Lyme is a multi-systemic disease. Lyme may present in a traditional way, with symptoms of joint pain, fevers, and a bulls-eye rash. Lyme disease may also present as emotional difficulties, memory loss, or extreme fatigue, without the presence of joint pain, or a bulls-eye rash. In children, Lyme can mimic ADHD or learning disabilities.
Studies have shown that people with Lyme disease may be misdiagnosed as other diseases including mood and anxiety disorders, heart problems, Lupus, Fibromyalgia, Chronic fatigue syndrome, Arthritis, and more. Some Lyme patients have been referred for psychiatric help. One clue that the cause of symptoms may be due to Lyme disease is that Lyme symptoms will often appear in a cyclical fashion. Every three to four weeks, symptoms may get worse and then return to their original pattern. Women may notice this cycle aligning with menstruation.
It is also important to diagnose co-infections. Ticks may transmit more than one disease in a single bite. Coloradans who remain ill after treatment for Lyme disease may have co-infections such as Anaplasmosis, Babesia, Bartonella, or others that require different or extended treatments.
Your medical care provider may not have experience in the diagnosis, testing or treatment for Lyme disease or co-infections, or may only treat a patient if they meet CDC surveillance criteria positive for disease. Some see Lyme as a simple infection easily cured by a short course of antibiotics. Others see it as a complex disease that requires comprehensive treatment. Naturopathic medical care providers may have alternative approaches to treatment of infection or may provide additional supportive care to boost immune function and repair cell damage.
It is okay to ask your medical practitioner about their training, and how they choose to diagnose and treat Lyme and other tick-borne diseases. It is your right as a patient to be informed that there is controversy regarding diagnosis, testing and treatment for Lyme disease and co-infections.
The CDC publishes treatment guidelines for Lyme disease that are consistent with the Infectious Disease Society of America, IDSA guidelines, leaving many physicians and patients that use the CDC as a resource unaware that there are differing professional guidelines authored by the International Lyme and Associated Diseases Society, ILADS available for the treatment of Lyme and other tick-borne diseases.
Colorado doctors are encouraged to attend physician trainings that offer additional perspectives and information to consider in contrast with the CDC/IDSA recommendations. This allows for informed clinical judgement and shared decision making with patients.
International Lyme and Associated Diseases Society (ILADS) provides a doctor referral system to help you locate an experienced care provider, Lyme Literate Medical Doctor (LLMD), as well as providing a wealth of information and resources to support Lyme patients, educators and physicians.
Lyme Disease Association, Inc. provides a doctor referral system to help you locate an experienced care provider as well as providing a wealth of information and resources to support Lyme patients, educators and physicians.
Lyme Disease.org provides a doctor referral system to help you locate an experienced care provider, provides both National and Colorado based support groups, hosts the largest Lyme patient registry MyLymeData, and publishes The Lyme Times that can assist in your pursuit of understanding Lyme and getting the care you need.
ProjectLyme.org provides a doctor referral system to help you locate an experienced care provider. They also host many patient/physician centered educational webinars and support.